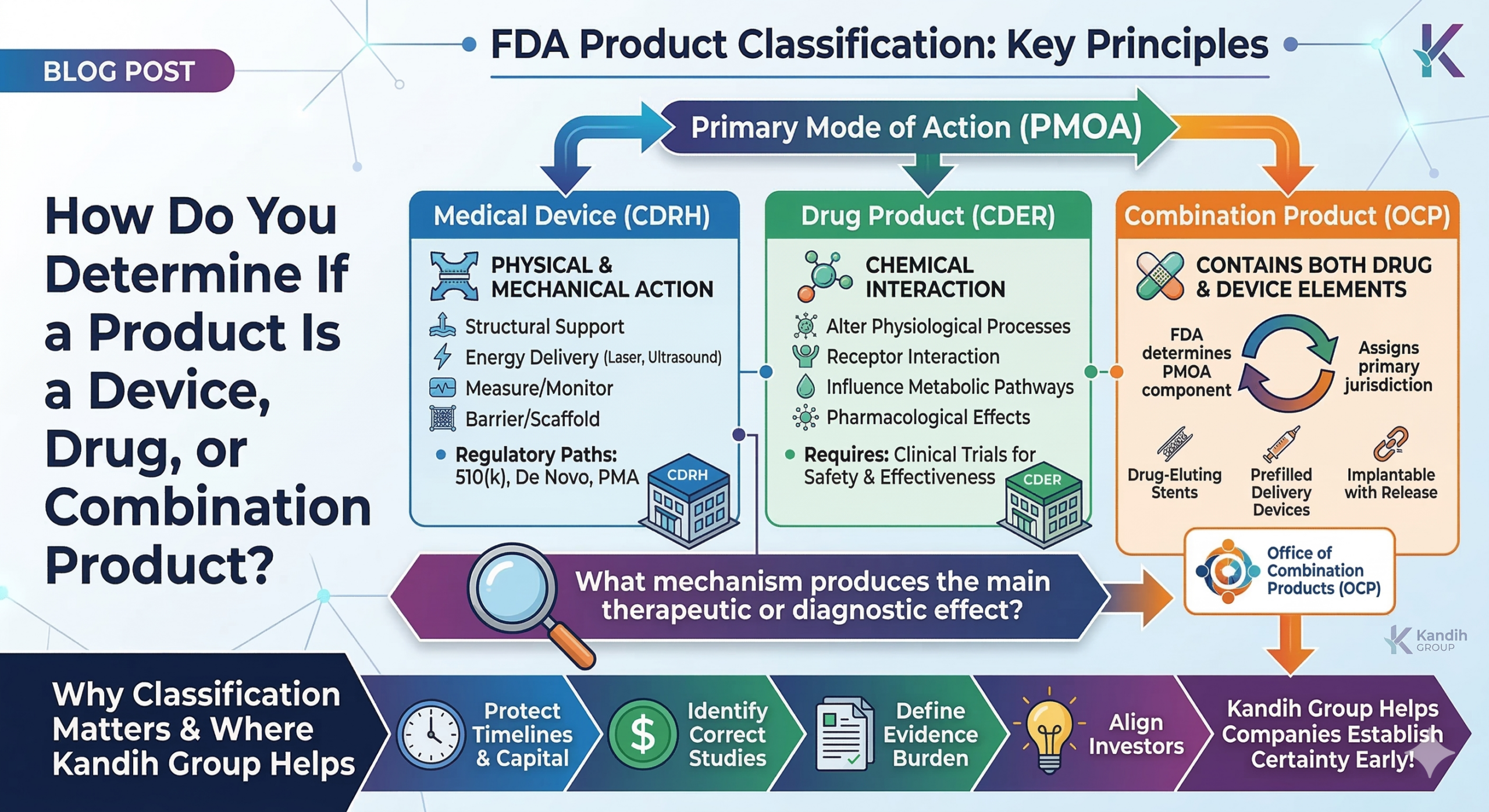
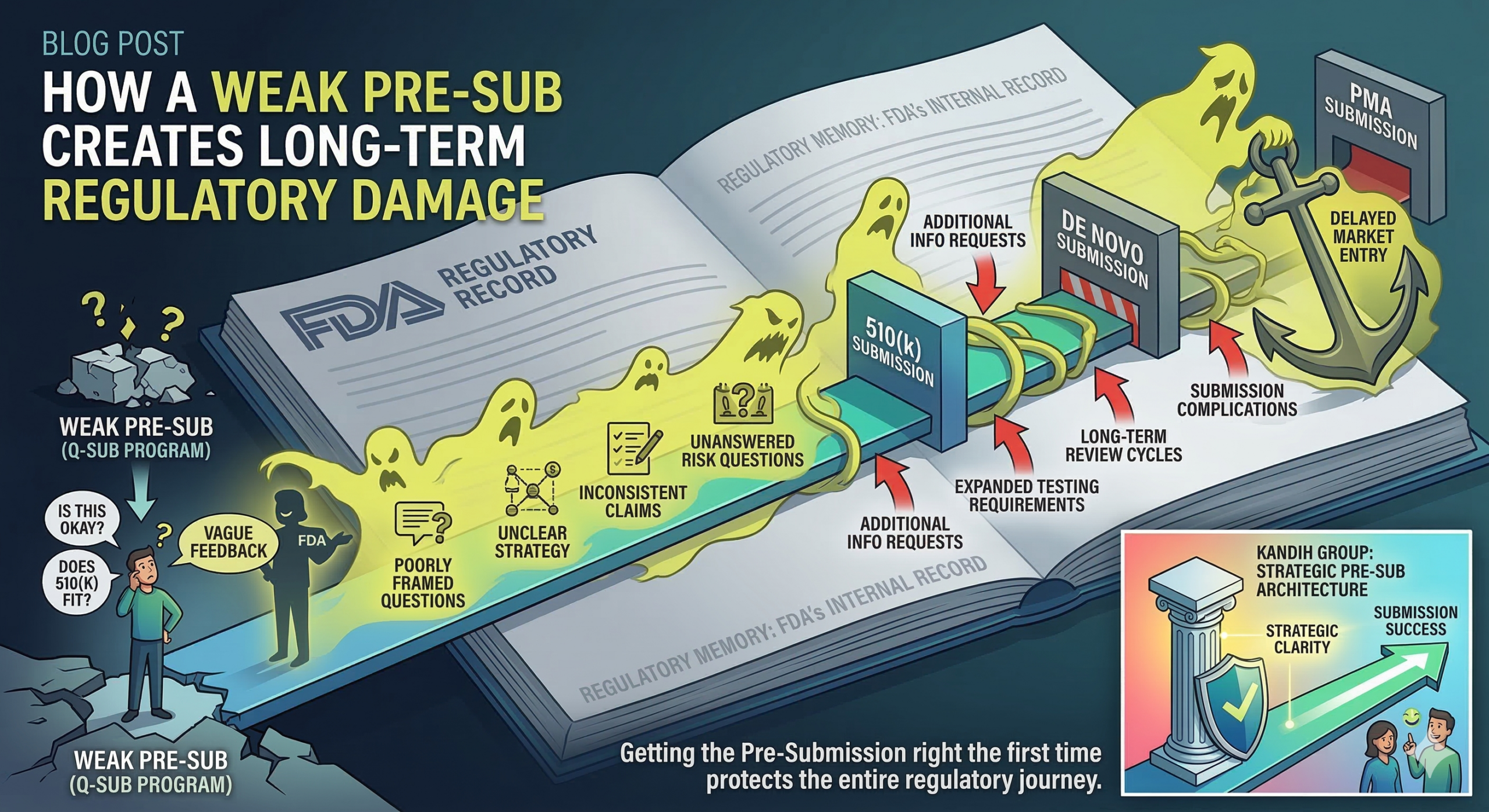
CAPA ≠ Paperwork. It’s a Risk-Control Feedback Loop

CAPA Failures as Evidence of a Broken Risk-Control System
January 13, 2026
Where Do Your CAPAs Originate Most?
January 15, 2026CAPA Survival Playbooks — Kandih Bioscience
One of the most common inspection surprises plays out the same way every time:
the CAPA file is immaculate—signed, dated, closed on schedule—yet the inspection ends with a Form 483.
That disconnect is not subtle. It reflects a fundamental misunderstanding of what CAPA is designed to do.
Many organizations still assume that a closed CAPA is a successful CAPA. From an inspection standpoint, that assumption is wrong. Closure only confirms task completion. It does not demonstrate that risk was controlled, recurrence prevented, or that management actually understood the problem they approved actions for.
Inspectors are not grading CAPA formatting. They are evaluating whether CAPA functions as a risk-control feedback loop—a system that detects signals, drives systemic correction, verifies effectiveness over time, and feeds learning back into the quality system. When CAPA is treated as paperwork, it becomes decoupled from real-world performance. That decoupling is exactly what inspectors are trained to detect.
This is not theory. It reflects how inspections unfold—on the floor, in conference rooms, and across records. If your CAPA system cannot demonstrate learning, control, and sustained improvement, documentation quality will not save it.
What FDA Actually Expects: A Regulatory Reality Check
From an inspection perspective, CAPA is not a standalone subsystem. It is the nervous system of the quality management framework.
Investigators typically begin with an operational signal—complaints, deviations, nonconformances, adverse events, OOS/OOT results, audit findings, or supplier failures. CAPA records are then examined to answer practical questions:
Was the signal detected appropriately?
Did the organization recognize when an issue crossed from isolated event to systemic risk?
Was risk interpreted correctly?
Was patient impact assessed realistically—or minimized to justify a narrow response?
Did the CAPA address the system, not just the symptom?
Were design controls, process capability, supplier controls, or quality oversight evaluated where relevant?
Was management actively involved?
Did leadership make informed decisions based on risk and data—or simply approve actions after the fact?
Inspectors test linkages deliberately. A complaint leads to design history files. A deviation leads to supplier qualification. A CAPA leads to management review trends. These are not random jumps; they reflect inspection logic centered on control and feedback.
This is why FDA does not treat CAPA as a QA task. QA may coordinate it, but inspectors evaluate CAPA as evidence of organizational learning and management control across the lifecycle.
Common CAPA Failure Modes (Inspector-Observed)
Across drugs, biologics, and devices, the same patterns recur.
1. Weak or Constrained Root Cause Analysis
Root cause is framed narrowly—often as human error—without evidence that systemic contributors were explored and ruled out.
Why it fails:
Incomplete causality means prevention is speculative. Inspectors read this as failure to understand risk pathways.
2. Training-Only or SOP-Only CAPAs
CAPAs rely on retraining or revised procedures without changes to process design, controls, or verification mechanisms.
Why it fails:
Training does not compensate for weak system design. FDA treats training-only CAPAs as evidence that risk architecture remains intact.
3. No Meaningful Effectiveness Verification
CAPAs close based on task completion. Effectiveness checks, if present, are immediate, qualitative, or disconnected from metrics.
Why it fails:
Effectiveness must be demonstrated over time. Without data, improvement is assumed—not proven.
4. CAPAs That Don’t Propagate Across Scope
An issue is fixed for one product, batch, line, or site despite plausible applicability elsewhere.
Why it fails:
Inspectors expect systemic thinking. Failure to assess scope signals blind spots in quality oversight.
5. Passive Management Review
CAPAs appear in management review as summaries, not decision points. Prioritization and resourcing are absent.
Why it fails:
Passive oversight equals loss of management control—regardless of meeting frequency.
CAPA Closure vs. CAPA Effectiveness: The Line Inspectors Care About
Administrative closure and regulatory effectiveness are not the same thing—and FDA draws that line clearly.
Administrative closure shows:
Actions were completed
Documentation requirements were met
Due dates were satisfied
CAPA effectiveness shows:
The risk no longer recurs
Performance metrics trend sustainably
The system behaves differently under similar conditions
Inspectors expect:
Time-based evidence (systems need time to stabilize)
Data-based verification (complaints, deviations, yield, OOS, KPIs)
Risk alignment (metrics tied directly to the failure mode)
Immediate closure after implementation is rarely credible for systemic issues. FDA understands variability—and expects firms to understand it too.
Business and Regulatory Consequences of Ineffective CAPAs
When CAPAs fail, the damage extends well beyond compliance.
Regulatory: 483s, warning letters, follow-ups, delayed approvals
Operational: Repeat deviations, disruptions, supplier instability
Strategic: Loss of inspection confidence, heightened scrutiny
Financial: Remediation costs, delayed revenue, valuation erosion
From FDA’s perspective, CAPA effectiveness is a proxy for whether an organization can manage risk without constant oversight. Once that confidence is lost, rebuilding it requires time—and evidence.
This is why investors, partners, and acquirers increasingly scrutinize CAPA performance. Weak CAPA systems signal operational fragility.
Anonymized Inspection Scenario
An investigator reviewed complaint trends tied to intermittent product failure. A CAPA had been opened, staff retrained, and the CAPA closed within 30 days.
When asked about effectiveness, the firm presented training records and stated that no further complaints had occurred. The investigator then reviewed complaint logs and identified similar events categorized differently after closure. No trend analysis had been performed. No upstream process or supplier review was documented.
The observation was not about documentation quality.
It was about failure to demonstrate sustained risk control and learning.
Inspector Red Flags (Quick Reference)
Inspectors become skeptical when they see:
CAPAs consistently closed faster than systems can stabilize
Repeated training-only actions across unrelated issues
Effectiveness checks without defined metrics or timelines
CAPAs disconnected from complaint or audit trends
Management review minutes without decisions
These are governance signals—not clerical issues.
What “Good” Looks Like in Practice
CAPA systems that withstand inspection share common traits:
Risk-based governance tied to patient impact and recurrence
Integrated data flow across complaints, deviations, audits
Outcome-based ownership, not task completion
Defined verification established upfront
Active management oversight visible in decisions
Many mature organizations use a simple internal test:
What risk was controlled?
How do we know it is controlled?
Over what timeframe?
Where else could this risk exist?
If those answers are not supported by data, the CAPA is not ready to close.
Strategic Takeaway
CAPA is not paperwork.
It is a risk-control feedback loop that signals whether an organization can learn, adapt, and protect patients over time. FDA evaluates CAPA effectiveness as evidence of management control, not administrative discipline.
For organizations preparing for inspection, growth, or diligence, objective CAPA gap analysis and inspection-readiness reviews identify vulnerabilities **before regulators—or partners—do.
References
Combination Products – CAPA & Investigations (21 CFR 4)
FDA expectations spanning 21 CFR 820 and 21 CFR 211.
https://www.gmp-compliance.org/gmp-news/warning-letter-on-combination-products-21-cfr-4
GMP-Compliance.org (2025)
Four Warning Letters Concerning CAPA and Root Cause Analysis.
SciLife.io (2025)
Worst FDA Warning Letters in Pharma: CAPA & CGMP Themes.
https://www.scilife.io/blog/worst-fda-warning-letters-pharma
Criticare Technologies, Inc. (2024)
Failure to establish and maintain CAPA procedures under 21 CFR 820.100(a); repeat deficiency.
Jiangsu Caina Medical Co., Ltd. (2024)
Inadequate CAPA procedures; failure to analyze quality data sources per 21 CFR 820.100(a)(1).
Sanofi (2025)
CGMP investigation and Quality Unit failures under 21 CFR 211; systemic CAPA expectations.