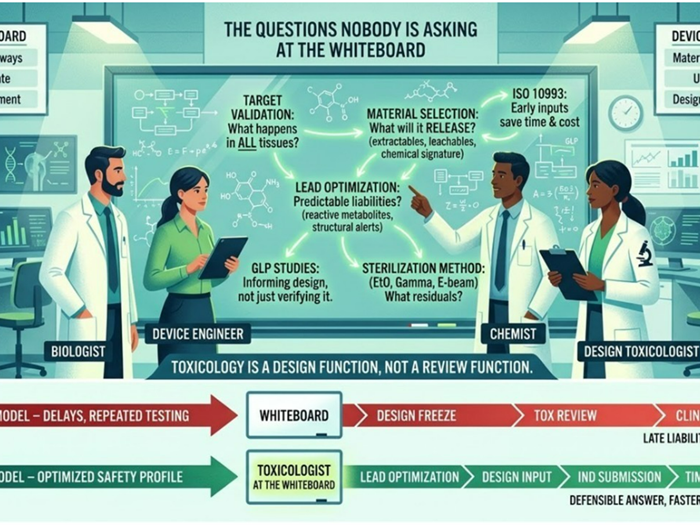
Breast Cancer & Toxicology: Why Exposures Matter as Much as Genetics

Aged Care and Toxicology: Protecting the Most Vulnerable
October 1, 2025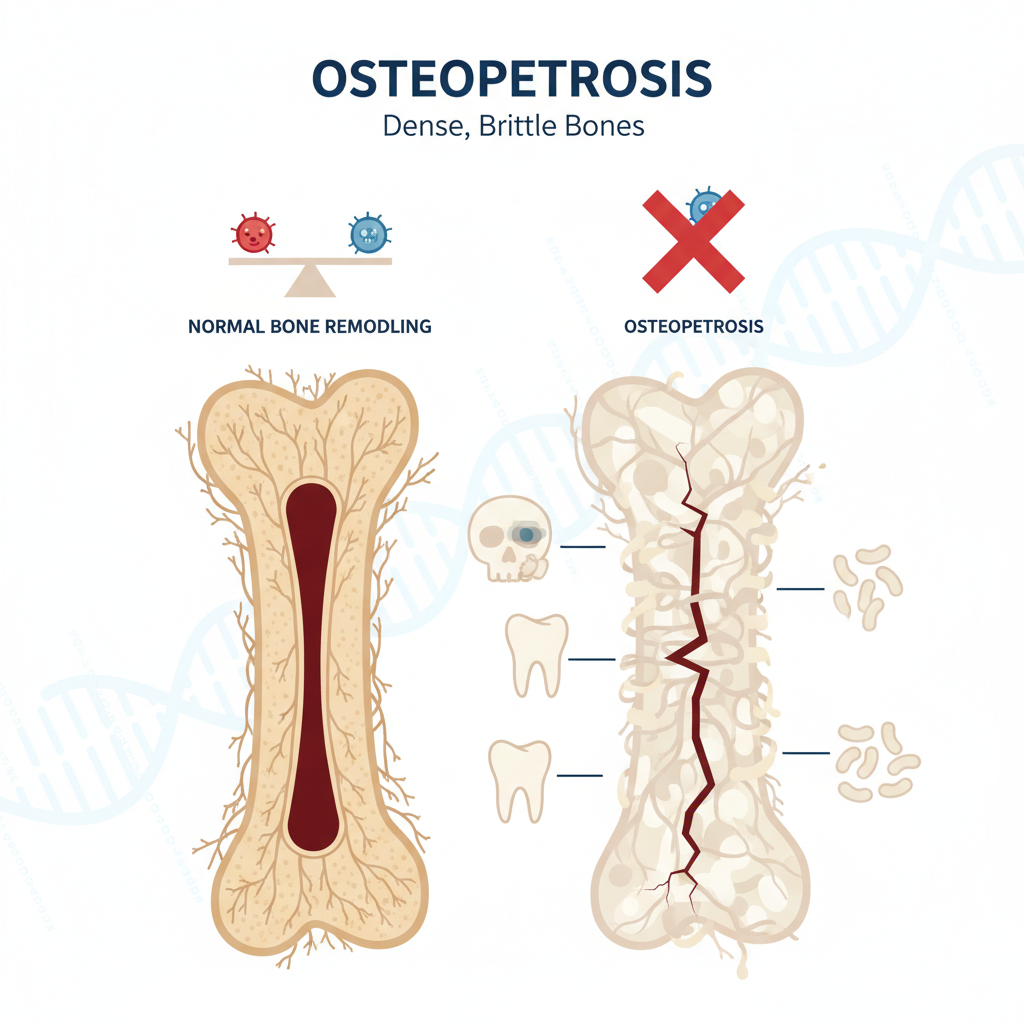
Osteopetrosis
October 3, 2025October is Breast Cancer Awareness Month, and most conversations focus on genetics, mammograms, and treatment advances. But there’s a blind spot: toxicology. Everyday exposures—from endocrine-disrupting chemicals in plastics to drug-induced toxicities during treatment—can shape both breast cancer risk and recovery.
If you’re a clinician, researcher, or public health leader, here’s the clear idea: you can’t talk about breast cancer prevention or survivorship without talking about toxicology.
Why Toxicology Belongs in the Breast Cancer Conversation
1. Environmental Risk Factors
Endocrine-disrupting chemicals (EDCs)—like BPA, phthalates, PFAS, and pesticides—can mimic estrogen and promote tumor growth. Decades of research show these exposures alter breast tissue biology and may increase cancer risk.
2. Drug-Induced Toxicities
Chemotherapy, hormone therapy, and targeted biologics save lives—but can also cause cardiotoxicity, hepatotoxicity, or even secondary malignancies. Toxicology defines safe dose limits, monitoring strategies, and protective interventions to balance efficacy with safety.
3. Cumulative Exposures
By midlife, many women carry layers of exposures—household chemicals, cosmetics, occupational hazards—that may interact with genetic predisposition or hormonal factors to amplify risk.
4. Vulnerable Windows
Toxicology reminds us that timing matters. Exposures during puberty, pregnancy, or menopause can have disproportionate effects on breast tissue, influencing both cancer initiation and treatment response.
Practical, Tactical Steps for Professionals
Integrate Exposure History into Care
Ask about occupational exposures, household chemicals, cosmetics, and supplement use during patient intake.
Support Safer Environments
Encourage reduced use of plastics in food storage, selection of fragrance-free personal care products, and avoidance of unnecessary pesticide contact.
Monitor for Treatment Toxicities
During chemotherapy or hormone therapy, track biomarkers of liver, kidney, and cardiac function. Adjust regimens early when toxic signals appear.
Educate on “Pinkwashing”
Many awareness products sold in October ironically contain chemicals linked to cancer risk. Use toxicology evidence to guide patients toward safer alternatives.
From Experience: Why This Matters
I’ve seen breast cancer survivors struggle with persistent fatigue and liver dysfunction long after completing chemotherapy. On deeper review, the cause wasn’t only the drugs—it was a combination of supplement interactions and environmental exposures that amplified chemotherapy’s hepatotoxic risks.
This is backed by evidence: studies have shown that complementary and alternative medicine (CAM) use, including herbal supplements, can interact with chemotherapy and increase toxicity if not monitored (Matthews et al., 2007).
By adjusting exposures—not just medications—patients experienced meaningful improvements in recovery and quality of life.
This is the power of toxicology: it widens the lens beyond genes and drugs to the full picture of risk.
The Bottom Line
Breast cancer isn’t only about genes or screenings—it’s about lifetime exposures and safety.
The clear idea: toxicology connects prevention, treatment, and survivorship by identifying risks medicine alone can’t solve.
For health leaders and clinicians, bringing toxicology into the breast cancer conversation means more comprehensive, safer, and smarter care.
References & Further Reading
1. Brody JG, Rudel RA. Environmental pollutants and breast cancer. Environ Health Perspect. 2003;111(8):1007–1019: https://pmc.ncbi.nlm.nih.gov/articles/PMC1241551
2. Soto AM, Sonnenschein C. Environmental causes of cancer: endocrine disruptors as carcinogens. Nat Rev Endocrinol. 2010;6(7):363–370: https://www.nature.com/articles/nrendo.2010.87
3. Armenian SH, et al. Cardiovascular disease among survivors of adult-onset cancer: a community-based retrospective cohort study. J Clin Oncol. 2016;34(10):1122–1130: https://pubmed.ncbi.nlm.nih.gov/26834065
4. U.S. Food & Drug Administration (FDA). Breast Cancer Drug Information: https://pmc.ncbi.nlm.nih.gov/articles/PMC10416257
5. Matthews H, et al. Herbal Medicines in Breast Cancer: Interactions and Safety Considerations. Breast Cancer Res Treat. 2007;104(3):299–306: https://pubmed.ncbi.nlm.nih.gov/40699761